Helen Ramscar
As all countries grapple with mathematical models, limited or inaccurate statistics and try to flatten exponential curves, citizens’ hopes are pinned on governments having an exit strategy to the Covid-19 crisis and the arrival of a safe vaccine. But some very challenging questions combining medical ethics and public policy remain to be answered before either outcome is a reality. Helen Ramscar poses some of these questions.
If all the HIV virus in the world was gathered together, it would fill one teaspoon.[1] When population figures are known for Covid-19, it may well be just one teaspoon too. That small. Yet the human cost combined with economic, political and societal damage in its first season is unprecedented in human history. And Covid-19 is not a pandemic that will pass in one wave. It is much more likely to involve a series of public health crises, requiring repeat lockdown measures and causing deep disruption well into 2021. The virus has moved rapidly across the world in the first three months of 2020, along the Silk Road and via international air travel. But as the first infected countries emerge gingerly by the summer of 2020 from their first lockdowns, other parts of the world will be in the grips of theirs. Despite the virus being a global threat, it is not a simultaneous global experience. As Covid-19 presents as a series of pulses across the world, and possibly doubling back repeatedly within countries, the problem of coordinating an international response will be challenging since the virus respects no borders or persons. Aligning public health responses, economic policies, the reopening of businesses (such as deciding when international air travel can responsibly be restarted, let alone key tourism industries) will require a new configuration of multilateral governmental cooperation or an international organisation with the infrastructure, credibility and legitimacy to act effectively and quickly. How will the international response play out?
It is hoped that Covid-19 will manifest as a series of diminishing, as opposed to escalating, waves; but it is too soon to say. There are clinical answers vital to government strategy that are still unknown, and yet governments have had to proceed with formulating policy without them. Until these questions can be answered, government policy is largely one of trial and error. And when the answers are known, some difficult aspects of medical ethics and public policy await.
Vaccine challenges
Mass testing. Until a vaccine is available, the question of natural immunity to Covid-19 is paramount. Blood tests can show the presence of antigens (here the presence of the virus) and antibodies (here the presence of natural immunity to the virus). Mass blood testing would provide clearer statistics to inform public policy. But if a person refuses the blood test, or is elderly or vulnerable and unable to provide consent, can and should the state forcibly draw blood from their veins?
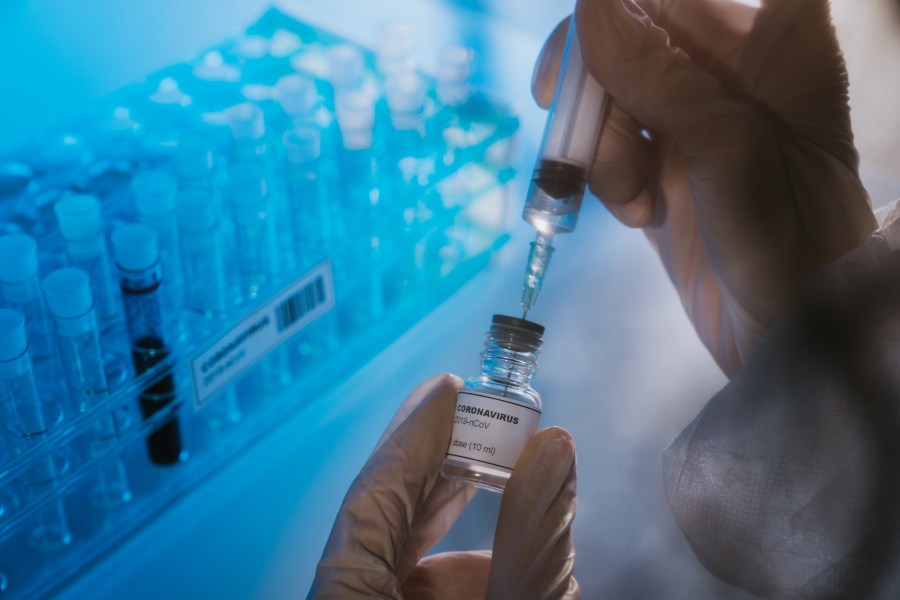
The sooner the better? Pharma is indicating that a Covid-19 vaccine could be available by spring 2021 (at the earliest). Established vaccines take many years in production, tested over lengthy safety trials before being licensed for public use. Is providing a fast-tracked vaccine a legitimate risk for governments to take?
Personal sovereignty. Pharma can produce very effective vaccines. But the anti-vaccine movement has grown significantly in recent years. When a vaccine becomes available which the government endorses, and individuals refuse to accept it for themselves or their children, what can and should the state do then?
Re-infection rates. At present there are suggestions in South Korea that some people who recovered from Covid-19 have been re-infected. This poses an extremely worrying situation whereby patients could be locked in a perpetual cycle of infection. If re-infection is occurring, this could make accelerating the process of producing a Covid-19 vaccine even more challenging. The vaccine dose required to provide enough immunity to overcome the prospect of re-infection could in turn make it a vaccine with nasty side effects. Ordinarily these would be tested over lengthy trials. If re-infection cases are confirmed, is a fast-tracked vaccine still an ethical option for governments to pursue? And if a government applies coercion to bring about a population-wide intervention on the grounds of public health, it needs to be sure the vaccine works. It otherwise risks expending essential moral capital in public health matters. The next time it tries to force an intervention, it would be a lot harder.
‘Vaccine diplomacy’. Whenever a vaccine becomes available, it will not be possible to roll it out to millions, possibly billions, of people simultaneously. Countries with factories that have done the most work to create the vaccine will expect to receive it first. It will be important that in reality and perception, distribution does not discriminate. How will vaccine diplomacy play out between the states who have it and those who need it?
Global public health activism. The climate change movement was reaching a crescendo in international public awareness and action by the end of 2019. This is likely to continue but alongside a new movement with undeniable global urgency and appeal. The 2020s look set to witness global public health as an international political and social grassroots movement that forces public health higher up the agenda of every country. Understanding and utilising ‘medical diplomacy’ to best effect will become an increasingly relevant aspect of international relations. How will states respond to perhaps a powerful grassroots call to international public health action? Would such a movement parallel the development of global environmentalism? If so, the way that ‘medical diplomacy’ and perhaps a new ‘vaccine diplomacy’ plays out in the 2020s will be a matter of some importance.
Helen Ramscar
Co-author of Tipping Point: Britain, Brexit and Security in the 2020s
Pingback: Vaccine Nationalism in the Age of Coronavirus, by Helen Ramscar – Tipping Point
Pingback: Vaccine Nationalism: The Ugly Face of Science and Politics - MetInfo